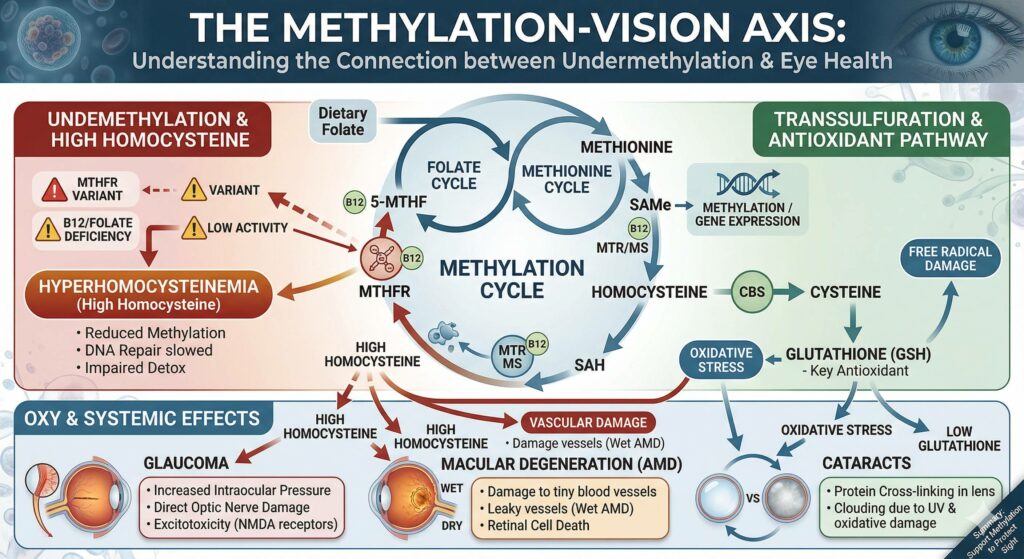
Research does suggest a significant link between “undermethylation” (and the genetic/biochemical factors that cause it) and the development of major eye conditions like glaucoma, macular degeneration (AMD), and cataracts.
The connection isn’t usually a straight line; rather, it’s a domino effect. When methylation is impaired, it often leads to high levels of homocysteine (a condition called hyperhomocysteinemia), which acts as a toxin to the delicate structures of the eye.
How Undermethylation Affects the Eyes
| Condition | The Methylation Connection | Mechanism |
| Glaucoma | Strongest link | High homocysteine can increase intraocular pressure and damage the optic nerve directly through oxidative stress. |
| Cataracts | Oxidative Stress | Impaired methylation reduces the body’s ability to produce antioxidants (like glutathione), leaving the lens vulnerable to “clouding” from UV and age. |
| Macular Degeneration | Vascular Health | Methylation is key for blood vessel integrity. Poor methylation can lead to inflammation and “leaky” vessels in the retina (Wet AMD). |
The Role of Homocysteine
If you are an “undermethylator,” your body likely struggles to convert homocysteine back into methionine. Excess homocysteine is particularly hard on the eyes because:
- Vascular Damage: It damages the tiny blood vessels that provide oxygen to the retina.
- Excitotoxicity: It can overstimulate neurotransmitter receptors (NMDA receptors) in the eye, leading to the death of retinal ganglion cells – a primary factor in glaucoma.
- Protein Cross-linking: In the lens, it can contribute to the “clumping” of proteins that creates cataracts.
Genetics and Nutrients
Many people who identify as undermethylators carry variants in the MTHFR gene (C677T or A1298C). These variants make it harder for the body to process folate and B12, which are the primary “fuel” for the methylation cycle.
Without enough methyl donors:
- DNA repair in ocular tissues slows down.
- Detoxification (via the glutathione pathway) is inhibited.
- Inflammation remains high, which is a known driver for both AMD and glaucoma.
Note: While the biochemical link is strong, eye health is also heavily influenced by lifestyle (smoking, UV exposure) and other genetic factors. If you’re concerned about your methylation status affecting your vision, it’s worth discussing homocysteine testing and methylated B-vitamin supplementation with a healthcare provider.
Ultimately, the “methylation-vision axis” serves as a powerful reminder that eye health is rarely an isolated issue, but rather a reflection of systemic biochemistry. By addressing undermethylation – particularly by managing homocysteine levels and supporting the MTHFR pathway – it is possible to reduce the oxidative and vascular strain that leads to chronic ocular conditions like glaucoma and AMD. Prioritizing these metabolic foundations provides a proactive strategy for preserving visual integrity and protecting the eyes from the cumulative damage of cellular stress.
Leave a Reply