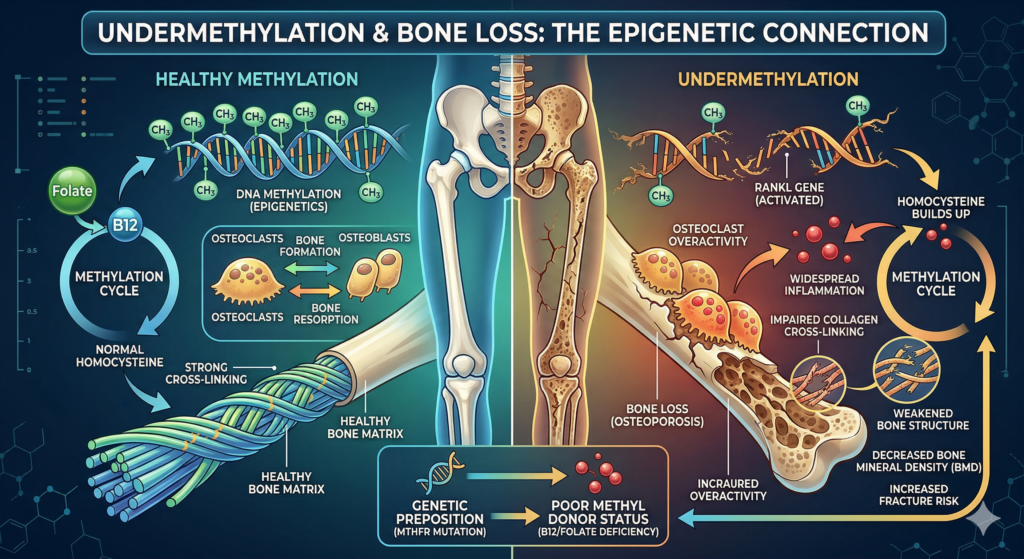
Does Under-Methylation cause bone loss?
Yes, undermethylation (or hypomethylation) can contribute to bone loss and an increased risk of osteoporosis. This happens through several biological pathways, most notably involving the buildup of homocysteine and the epigenetic regulation of bone cells.
The link between poor methylation and bone health is primarily driven by three factors:
1. The Homocysteine Connection
In a state of undermethylation, the body often struggles to convert homocysteine back into methionine. This leads to elevated homocysteine levels (hyperhomocysteinemia), which is a well-documented risk factor for bone loss.
- Collagen Weakening: Homocysteine interferes with the “cross-linking” of collagen fibers. Since collagen provides the flexible “rebar” that keeps bones from being brittle, this interference makes the bone matrix structurally weaker, even if density looks normal on a scan.
- Reduced Blood Flow: High homocysteine can damage small blood vessels (microvasculature) within the bone, depriving bone tissue of necessary nutrients and oxygen.
2. Epigenetic “Switching” (DNA Methylation)
Methylation acts like a “mute” button for certain genes. When you are undermethylated, that mute button isn’t pressed, allowing specific genes to become overactive:
- RANKL Overexpression: Research shows that hypomethylation (lack of methyl groups) on the promoter of the RANKL gene causes it to stay “turned on.” RANKL is a protein that stimulates osteoclasts – the cells responsible for breaking down and resorbing bone.
- Osteoclast Overactivity: When RANKL is too active, bone is broken down faster than the body can rebuild it (osteoblast activity), leading to a net loss of bone mineral density.
3. Nutritional Deficiencies
Undermethylation is frequently tied to deficiencies in key B vitamins that serve as methyl donors. These vitamins have independent roles in bone health:
- Vitamin B12 & Folate: Low levels of these vitamins are strongly correlated with lower bone mineral density and a higher risk of hip fractures.
- MTHFR Mutations: Genetic variants like MTHFR C677T can lead to undermethylation. Studies have shown that individuals with these variants may have a higher susceptibility to osteoporosis, particularly when their intake of folate and B12 is low.
Summary Table: Methylation and Bone Health
| Mechanism | Impact of Undermethylation | Result |
| Homocysteine | Increases (Hyperhomocysteinemia) | Weakens collagen & bone matrix |
| RANKL Gene | Hypomethylated (Unsilenced) | Increases bone-destroying cells |
| Osteoblasts | Reduced activity/differentiation | Slower new bone formation |
| Vitamin Co-factors | B12, Folate, and B6 are often low | Decreased bone density |
How to Monitor
If you are concerned about undermethylation affecting your bones, common clinical markers to check include:
- Homocysteine (Plasma): Ideally kept below 8.0 or 9.0 umol/L for optimal bone and cardiovascular health.
- Serum B12 & Folate: To ensure the methylation cycle has the necessary raw materials.
- DEXA Scan: To measure actual bone mineral density.
Ultimately, bone health is about much more than just calcium and Vitamin D; it is a delicate balance of cellular signaling and biochemical recycling. Addressing undermethylation allows you to tackle the biological root causes of bone degradation – like elevated homocysteine and overactive bone-resorbing cells – rather than just managing the symptoms of bone loss. By supporting your body’s methylation cycle through targeted nutrition and lifestyle adjustments, you aren’t just reinforcing your skeletal frame; you’re optimizing the epigenetic “software” that governs your long-term vitality. Always consult with a healthcare professional to tailor a plan to your specific metabolic needs.

Leave a Reply