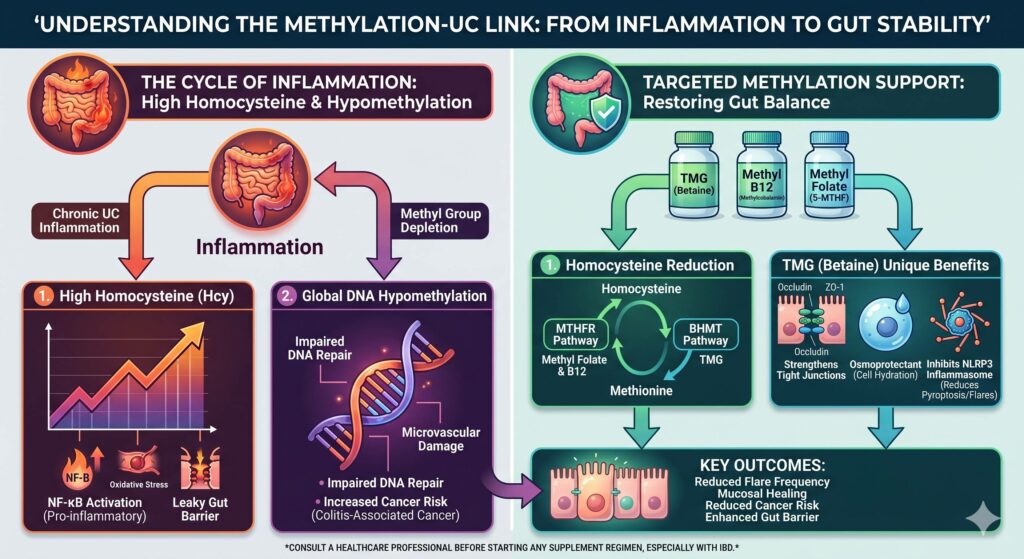
Research into the relationship between Ulcerative Colitis (UC) and methylation suggests a significant, though complex, link. While “under-methylation” is often used as a broad term in functional medicine, clinical research specifically identifies global DNA hypomethylation (a lack of methyl groups) in the colonic tissue of patients with chronic UC.
Does UC Indicate Possible Under-Methylation?
Yes, there is a recognized connection. Studies have shown that the rectal and colonic mucosa of people with UC often exhibit hypomethylation.
- Cause vs. Effect: It is currently debated whether poor methylation helps trigger UC or if chronic inflammation depletes methyl donors. Continuous cell turnover in the gut (due to inflammation) creates a high demand for methyl groups to repair DNA.
- Cancer Risk: One of the most critical aspects of this link is that hypomethylation in the colon is a known precursor to Colitis-Associated Cancer (CAC). When DNA isn’t properly methylated, certain “silencing” mechanisms fail, potentially leading to the over-expression of genes that promote tumor growth.
Would Boosting Methylation Help?
Supplementing with Methyl B12, Methyl Folate, and TMG (Trimethylglycine) is a common strategy to support the body’s “one-carbon metabolism.” While these are not a “cure” for the autoimmune aspect of UC, they may help manage the disease in several ways:
1. Methyl Folate & Colorectal Cancer Prevention
Folate is the most studied supplement in this context. Many UC medications (like sulfasalazine) are folate antagonists that block absorption.
- The Benefit: High-dose folate has been shown in several meta-analyses to significantly reduce the risk of colorectal cancer in UC patients by supporting proper DNA methylation.
- Methylated Form: Using L-methylfolate (5-MTHF) is often preferred because it bypasses the MTHFR enzyme pathway, which can be sluggish in some individuals.
2. TMG (Betaine) and Gut Barrier Integrity
Recent studies (including research from 2022-2026) have highlighted TMG’s role beyond just being a methyl donor.
- Inflammasome Inhibition: TMG has been shown to inhibit the NLRP3 inflammasome, a protein complex that triggers “pyroptosis” (inflammatory cell death) in the gut lining.
- Tight Junctions: TMG acts as an osmoprotectant, helping intestinal cells stay hydrated and strengthening “tight junction” proteins like occludin and ZO-1. This helps reduce “leaky gut” symptoms often associated with UC.
3. Methyl B12 and Homocysteine
UC patients often have elevated levels of homocysteine, a marker for poor methylation and a risk factor for blood clots (which are more common in IBD patients).
- The Pathway: Methyl B12 and Methyl Folate work together to convert homocysteine back into methionine:
- Homocysteine + 5-Methyl-THF –> MTR Methionine
- TMG’s Role: TMG provides a “backup” pathway for this recycling via the BHMT enzyme, which is particularly active in the liver and kidneys.
Summary Table: Methylation Support in UC
| Supplement | Primary Role in UC | Clinical Significance |
| Methyl Folate | DNA Methylation & Repair | Strong evidence for reducing colon cancer risk. |
| Methyl B12 | Homocysteine Regulation | Helps prevent anemia and reduces blood clot risk. |
| TMG (Betaine) | Osmoprotectant & Anti-inflammatory | Protects the gut barrier and inhibits the NLRP3 inflammasome. |
Important Considerations
- The “Over-methylation” Risk: Taking high doses of methyl donors can sometimes lead to side effects like anxiety, insomnia, or irritability in sensitive individuals.
- Flare Activity: During an active flare, the priority is typically reducing acute inflammation (often via biologics or steroids) before the body can effectively utilize these building blocks for repair.
Does High Homocysteine Levels Increase the Occurrence of Ulcerative Colitis?
The relationship between homocysteine (Hcy) and Ulcerative Colitis (UC) is a “two-way street” where elevated levels both result from the disease and actively drive its progression. Current research (2024-2026) suggests that managing these levels is a critical strategy for stabilizing the gut.
Does High Homocysteine Increase UC Occurrence and Severity?
Yes. While it was previously thought that high homocysteine was merely a side effect of malabsorption in IBD, current evidence identifies it as a pro-inflammatory trigger that exacerbates the disease.
- Pro-Inflammatory Signaling: Elevated Hcy acts as a signaling molecule that activates NF-κB, a master switch for inflammation. This leads to the overproduction of COX-2 and PGE2 (prostaglandin E2), which directly attack the colonic mucosa.
- Microvascular Damage: High Hcy promotes “microthrombi” (tiny blood clots) in the small blood vessels of the gut. This restricts oxygen and nutrient flow to the intestinal lining, making it harder for the gut to heal and more prone to ulceration.
- Oxidative Stress: Hcy increases the production of reactive oxygen species (ROS), which damages the DNA of colon cells. This is why chronic high Hcy is linked to an increased risk of colitis-associated cancer.
Can TMG (Betaine) Reduce UC Flare-ups?
Preclinical and emerging clinical data suggest that TMG (Trimethylglycine) can be highly effective in reducing the frequency and severity of flare-ups through three distinct mechanisms:
1. The Homocysteine “Drain”
TMG provides the most direct way to lower Hcy in the liver and kidneys via the BHMT (Betaine-Homocysteine Methyltransferase) pathway. By converting Hcy back into Methionine and subsequently SAMe, TMG:
- Reduces the “fuel” for intestinal inflammation.
- Restores the body’s primary methyl donor (SAMe), which is essential for DNA repair in the gut lining.
2. Strengthening the “Tight Junctions”
One of TMG’s most potent roles in UC is as an osmoprotectant. UC flares are characterized by a “leaky gut” where the barrier fails.
- Barrier Support: TMG has been shown to upregulate key barrier proteins like Occludin and ZO-1.
- Hydration: It helps intestinal cells maintain their volume and hydration under the stress of inflammation, preventing cell death (apoptosis).
3. Inhibition of the NLRP3 Inflammasome
Recent studies (2025-2026) highlight TMG’s ability to block the NLRP3 inflammasome. This is a protein complex that, when overactive in UC patients, triggers pyroptosis – a highly inflammatory form of cell death that causes the classic “explosive” flares and mucus production.
Recommended Strategy for Methylation Support
To effectively use these nutrients for UC management, they are typically used in combination to cover all “one-carbon” pathways:
| Nutrient | Target | Role in Flare Prevention |
| TMG (Betaine) | BHMT Pathway | Lowers Hcy; protects gut barrier; anti-pyroptosis. |
| Methyl Folate | MTHFR Pathway | Essential for DNA synthesis; reduces cancer risk. |
| Methyl B12 | Methionine Synthase | Works with folate to recycle Hcy; supports nerve/blood health. |
Practical Note
While TMG is generally well-tolerated, it is a powerful methyl donor. In some individuals, “boosting” methylation too rapidly can cause a temporary increase in GI transit time or mild anxiety. Starting with a lower dose (e.g., 500mg) and titrating up to 1,500mg–3,000mg is a common approach in functional protocols.
Research into Ulcerative Colitis (UC) highlights a critical link between chronic gut inflammation and DNA hypomethylation. When the colonic mucosa lacks sufficient methyl groups, the body struggles to regulate gene expression, leading to the over-activation of pro-inflammatory pathways like NF-kB. This deficiency is further complicated by elevated homocysteine levels, which act as a signaling molecule for oxidative stress and microvascular damage. High homocysteine not only exacerbates the severity of flares by restricting oxygen flow to the intestinal lining but also significantly increases the long-term risk of colitis-associated cancer by impairing DNA repair mechanisms.
To counter these effects, a combination of Methyl B12, Methyl Folate, and TMG (Trimethylglycine) offers a systemic approach to restoring gut stability. While Methyl B12 and Folate primarily target the recycling of homocysteine through the MTHFR pathway, TMG provides a distinct advantage by acting as an osmoprotectant. TMG strengthens the “tight junction” proteins that maintain the gut barrier and inhibits the NLRP3 inflammasome, a protein complex responsible for the inflammatory cell death seen during acute flares. Together, these nutrients help reduce the pro-inflammatory load, support the structural integrity of the colon, and provide the biochemical building blocks necessary for mucosal healing.


Leave a Reply