Fatty liver disease – specifically Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD, formerly NAFLD) – is a condition where excess fat builds up in liver cells. It is increasingly common and closely tied to metabolic health and nutritional status.
Causes of Fatty Liver Disease
The development of a fatty liver is typically a multi-step process involving metabolic stress:
- Insulin Resistance: When cells stop responding to insulin, the body sends more free fatty acids to the liver, and the liver itself begins to produce more fat.
- Dietary Excess: High intake of processed carbohydrates and fats, beyond what the body can burn for energy.
- Oxidative Stress: Damage to liver cells from reactive oxygen species, often triggered by toxins, poor diet, or chronic inflammation.
- Genetics: Specific gene variants (like PNPLA3) can make some individuals more prone to storing liver fat regardless of diet.
The Link to Under-Methylation
There is a significant biochemical link between the methylation cycle and liver health. The liver is the primary hub for methylation, and “under-methylation” can directly contribute to fat accumulation:
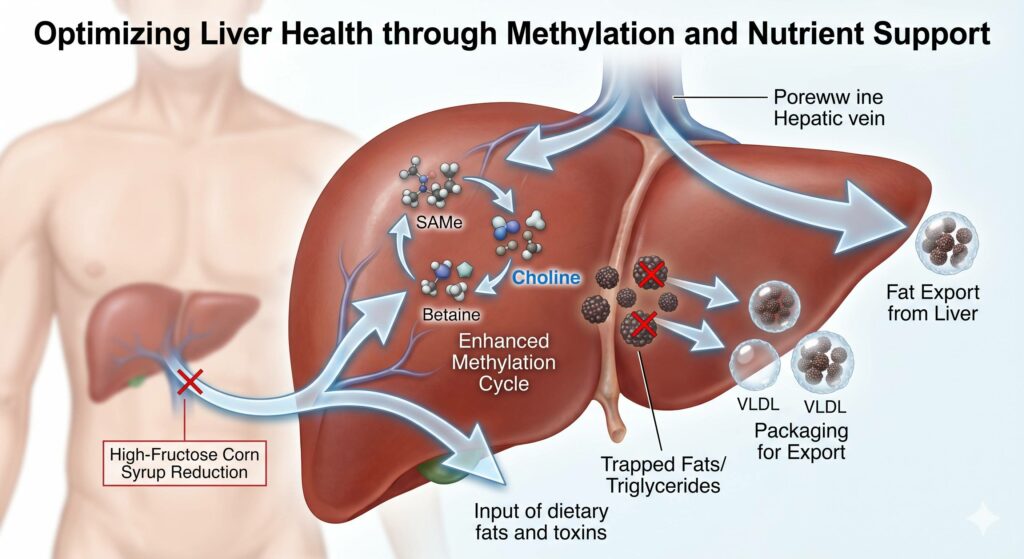
- The PEMT Pathway: The enzyme PEMT (Phosphatidylethanolamine N-methyltransferase) converts phosphatidylethanolamine into phosphatidylcholine (PC). This process requires three molecules of SAMe (the body’s universal methyl donor).
- VLDL Export: The liver needs phosphatidylcholine to “package” triglycerides into Very Low-Density Lipoproteins (VLDL). If you are under-methylating, you may not produce enough PC.
- The Result: Without enough PC to package the fat for export, the fat becomes “trapped” in the liver, leading to steatosis (fatty liver).
Reversing Fatty Liver
In many cases, fatty liver is reversible, especially in the early stages, through targeted lifestyle and nutritional shifts:
Reducing High Fructose Corn Syrup (HFCS)
Reducing HFCS is one of the most effective ways to combat liver fat. Unlike glucose, which every cell in the body can use, fructose is processed almost exclusively by the liver. When the liver is overwhelmed by high amounts of fructose, it converts the sugar directly into fat through a process called de novo lipogenesis.
The Role of Choline
Choline is an essential nutrient for liver function. It acts as a precursor to phosphatidylcholine.
- Clinical Evidence: Choline deficiency is a well-documented cause of fatty liver.
- Synergy: Adding choline (or its metabolites like TMG/Betaine) provides the building blocks necessary for the liver to export fat. TMG can also “spare” choline by providing methyl groups directly to the homocysteine-to-methionine path.
Physical Activity
Both aerobic exercise and resistance training improve insulin sensitivity and help the body “burn” through the glycogen and fatty acids stored in the liver.
Herbs and Nutrients for Liver Support
Several botanicals and compounds have been studied for their ability to reduce liver fat and inflammation:
- Milk Thistle (Silymarin): Perhaps the most well-known liver herb, it acts as an antioxidant and may help stabilize liver cell membranes to prevent toxin-induced damage.
- Turmeric (Curcumin): High-potency curcumin may help reduce liver fat and lower inflammatory markers associated with MASLD.
- Berberine: Often used for blood sugar management, berberine has shown significant potential in clinical trials for reducing liver fat by improving insulin sensitivity.
- N-Acetyl Cysteine (NAC): A precursor to glutathione, the body’s master antioxidant, which helps the liver neutralize oxidative stress.
- Dandelion Root: Traditionally used as a cholagogue to stimulate bile flow, which assists in the digestion of fats and overall detoxification.
Fatty liver disease, or MASLD, primarily stems from metabolic stressors like insulin resistance and chronic dietary excess, which force the liver to store rather than process lipids. A critical yet often overlooked factor is the role of the methylation cycle; specifically, the liver requires methyl donors to produce phosphatidylcholine, a necessary component for “packaging” fats into Very Low-Density Lipoproteins (VLDL) for export. When methylation is compromised – often termed “under-methylation” – the liver loses its ability to move these fats out of its cells, leading to a localized buildup, oxidative stress, and chronic inflammation.
Reversing this condition involves a targeted approach to reduce metabolic load and restore biochemical balance. Eliminating high fructose corn syrup is paramount, as the liver converts fructose directly into fat through de novo lipogenesis, bypassing many of the body’s natural metabolic brakes. Concurrently, increasing choline intake provides the essential precursors needed for fat export, while adding methyl-sparing nutrients can optimize the entire cycle. Complementary herbal supports, such as Milk Thistle, Curcumin, and Berberine, further aid the process by neutralizing free radicals, stabilizing cell membranes, and improving insulin sensitivity to facilitate long-term liver recovery.


Leave a Reply